Howdy Readers! Today I wanted to take some time to report on a case that I was presented with during this previous basketball season. Then I will discuss how I addressed the case and what I wish that I could have changed about the case. I will also be using my findings from the patient's Selective Functional Movement Assessment (SFMA), and so here is the SFMA acronym legend:
FN: Functional & Non-painful
FP: Functional & Painful
DN: Dysfunctional & Non-painful
DP: Dysfunctional & Painful
Background:
A 21 year old NCAA division III basketball player was competing in a JV basketball game when he suffered a direct blow to the low back by an opposing player's elbow. The supervising athletic trainer (I was busy prepping the varsity team to play) determined there were no gross deformities, ruled out neurological involvement (dermatomes & myotomes WNL), and ruled out any potential fractures. Nevertheless, the player was unable to return to play and finish the game due to pain.
This player had a previous history of catastrophic injury as a high school basketball player when he was undercut by an opponent. He fell on his upper back and hit his head suffering a fractured scapula and traumatic brain injury that lead to him being placed into a medically-induced coma. Additionally, he had a history of low-back pain during high school. The year previous to the current incident this athlete suffered a season-ending concussion as well.
After the game was over this athlete returned to his hometown with his parents. The parents and the athlete planned to see a family friend that is an orthopaedic surgeon in the following days. Upon consulting with the doctor it was revealed to the athlete that he had degenerative joint disease (DJD) in his lumbar spine and he was sent back to me for rehabilitation at my discretion.
Upon hearing this I definitely began to dismiss the DJD because I knew that suffering an elbow to the low back in one game of basketball didn't give this player DJD. I began to talk with the patient about pain science, how it didn't matter if he had DJD because he had it before when he was pain-free, and how we weren't going to attempt to change it. I did discuss how we would perform an SFMA and evaluate in which patterns he was moving dysfunctionally & why they were dysfunctional.
Assessment:
SFMA Top Tier Results & Breakout Findings--
Cervical Flexion = DN: Tissue Extensibility Dysfunction
Cervical Extension = FN
Cervical Rotation = Left - FN / Right - DN: (Tissue Extensibility Dysfunction)
Upper Extremity Pattern 1 = DN (Bilaterally, Left worse than Right): (Functional Shoulder Pattern Stability/Motor Control Dysfunction)
Upper Extremity Pattern 2 = FN (Bilaterally)
Multi-Segmental Flexion = DP (Posterior Chain Tissue Extensibility Dysfunction)
Multi-Segmental Extension = DN: (Thorax Extension Stability/Motor Control Dysfunction, Hip Extension Tissue Extensibility Dysfunction)
Multi-Segmental Rotation = DN (Fundamental Rotational Pattern Stability/Motor Control Dysfunction, Hip ER Tissue Extensibility Dysfunction)
Single Leg Stance = DN (Lower Posterior Chain Tissue Extensibility Dysfunction)
Overhead Deep Squat = DN (Hip and Lower Leg Posterior Chain Tissue Extensibility Dysfunction)
Plan:
Based upon my SFMA findings I decided to attack the greatest areas of dysfunction first. I determined that the hip flexion/posterior chain TED (~40 degrees passive SLR), and cervical flexion & rotation were the patient's greatest limitations. This is what I formulated my initial treatment plan around as well. I began with an easy 5 minute warm-up on a stationary bike followed by some instrument assisted soft tissue mobilization (IASTM) to the posterior neck, proximal hamstrings attachment near the ischial tuberosity and distal attachment of the biceps femoris to prepare for some Muscle Energy Technique (MET).
Day 1: Pain (7/10)
 |
| Upper Trap MET |
I performed MET techniques (redundancy?) for the upper trap, scalenes, and posterior neck extensors. I performed 3 sets of autogenic isometric inhibition on the right side and an extra set on the left side. This brought cervical flexion and rotation to FN immediately following application of the MET treatment.
I then instructed the patient to perform a couple sets of supine kettlebell carries. Each set lasted until the patient neared fatigue and was unable to retract and "pack" the shoulder/scapula. This was performed bilaterally. Reassessing the upper extremity pattern 1 revealed decreased winging compared with baseline.
 |
| MET for the Scalenes |
 |
| Before Treatment |
Next, I performed MET for the posterior hamstrings. Specifically, I also instructed the patient on performing an autogenic isometric inhibitory technique. I performed this bilaterally and found that the patient's passive SLR increased ~20 degrees immediately by the end of treatment.
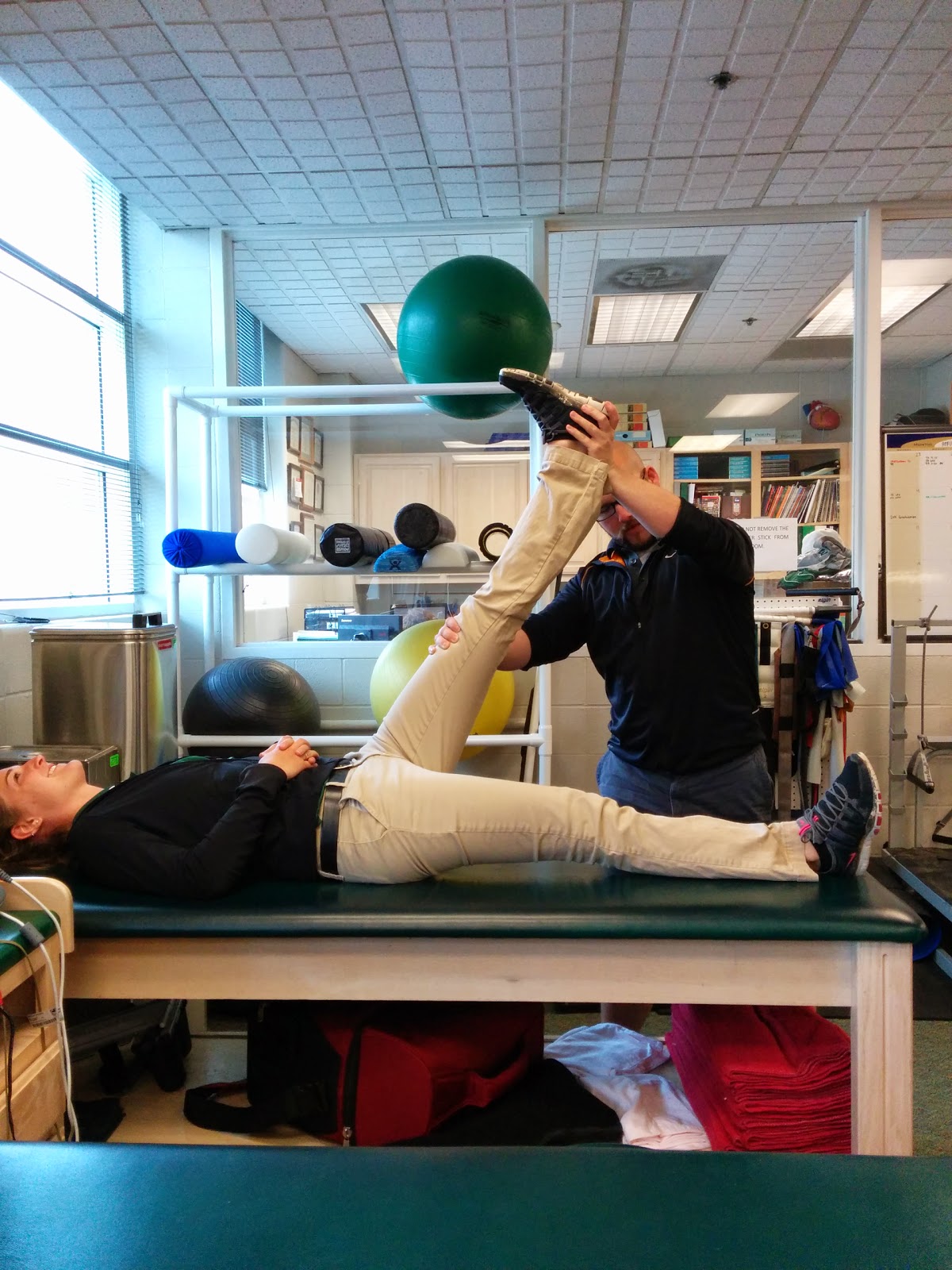 |
| After Treatment |
The patient was unable to attempt rolling exercises due to passive back pain so instead of attempting to restore rolling I had the patient perform some light stretching hip external rotation and calf stretching after having their glutes and gastroc/soleous worked out using a rolling stick by my student.
 |
| Easy Hip ER Stretch |
 |
| Straight Leg Gastrocnemius Stretch - Towel prevents pronation |
 |
| Bent Knee Soleus Stretch - Towel prevents pronation again |
Day 2: Pain (4/10)
The patient returned the second day with increased cervical flexion and rotation patterns but they were no longer functional. I repeated the previous days IASTM and MET techniques and once again these patterns were FN after application. In attempt to prolong these gains, I applied some Rock Tape to the upper traps and scalenes. Once again I had the patient do some kettlebell carries while in a supine position.
The passive SLR was still increased from the previous day but was still about 15 degrees short of normal. The patient was able to foam roll without increased pain and so I had him foam roll the entire posterior leg chain before IASTM to the aforementioned patterns. Again, we used the previous day's MET application to the hamstrings and this increased the passive SLR to normal.
Due to the patient's ability to have such drastic increases in mobility in such a small amount of time I suspected crucial core stability issues. In attempt to progress this patient quickly I wanted to restore rolling ASAP for the supine to prone upper extremity rolling pattern. I spent about 15 minutes working on rolling with him before calling it a day. Rolling was definitely not perfect but was much better than when we began.
Day 3: No Pain?
On the third day of treatment the athlete returned with FN cervical flexion, and rotation patterns and now Multi-Segmental Flexion was a DN. The athlete reported being sore in the shoulders and hips but no longer was experiencing any pain. We were now about 7 days out from initial injury. I continued to work on rolling patterns and was able to progress to some quadruped and tall-kneeling exercises before the day's end. I could tell that the athlete was very excited to return to basketball so I began his RTP progress with some easy free-throw shooting.
Return to Play and Further Treatment:
Unfortunately, the next day the athlete returned home for spring break and was no longer under my supervision. Despite my best efforts to provide a substantial home-exercise program for this athlete he was so enthused by his progress that he did not stick to his HEP and instead played basketball and rested his entire break.
Upon returning to school the athlete was no longer compliant with his rehab despite the presence his many dysfunctional movement patterns (MSF, MSE, UE #1, MSR, SLS, ODS) and would no longer come for rehab. Reluctantly, I continued to let him participate in practice and JV games. It wasn't because I didn't care about making him better but more because of it being an issue of me being stretched too thin between other athletes that had issues and wanted my help and patients like him that needed my help but wanted none of it because they no longer suffered. It is not an ideal situation but it is the way the world works sometimes. Ideally for me I wish I had been in a position where there was somebody(like a strength coach) that was familiar with the FMS and corrective exercises to help these athletes overcome their dysfunction.
Points of Distinction & Conclusion:
What I thought was interesting regarding this case was the patient's history of traumatic injury to the left scapula and the presence of ipsilateral hypertonic neck muscular and poor scapular stability when compared bilaterally. I do not know if this was present since his previous injury but its hard for me to ignore such a glaring "coincidence" when I see it. When I initially worked with this athlete I had a little contempt for the incomplete rehabilitation that he must have been put through following his previous injuries.
However, I soon began to feel and conclude that much of this could have been the athlete's own doing and not that of previous clinicians. I even tried the route of touting injury prevention, performance enhancement and how he may be a ticking-time bomb for re-injury and recurrence of back pain. Some people, patients, and athletes just do not seem to want help unless they are physically writhing in pain and unable to walk. I am not sure if this is pride or pure laziness!









































.gif)
.JPG)

